Rh Incompatibility I Hemolytic Disease of the Newborn
- 2. INTRODUCTION Rh incompatibility is a condition that occurs during pregnancy if a woman has Rh-negative blood and her baby has Rh-positive blood.
- 3. DEFINITION Rh disease (also known as rhesus isoimmunisation, Rh (D) disease, rhesus incompatibility, rhesus disease, RhD hemolytic disease of the newborn, rhesus D hemolytic disease of the newborn or RhD HDN) is a type of hemolytic disease of the newborn (HDN). The disease ranges from mild to severe, and typically occurs only in some second or subsequent pregnancies of Rh negative women where the fetus's father is Rh positive, leading to a Rh+ pregnancy.
- 4. CAUSES A difference in blood type between a pregnant woman and her baby causes Rh incompatibility. The condition occurs if a woman is Rh-negative and her baby is Rh-positive.
- 5. RISK FACTORS This may have happened during: An earlier pregnancy (usually during delivery). An ectopic pregnancy, a miscarriage, or an induced abortion. (An ectopic pregnancy is a pregnancy that starts outside of the uterus, or womb.) A mismatched blood transfusion or blood and marrow stem cell transplant. An injection or puncture with a needle or other object containing Rh-positive blood.
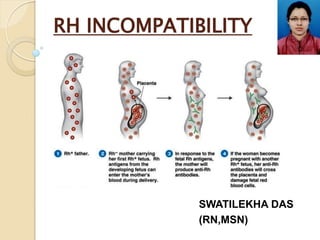
- 6. PATHOPHYSIOLOGY Rh Incompatibility in Pregnancy- 1st Pregnancy Father (RhD+) Mother (RhD-) Fetus (RhD+) first newborn(RhD+)Safe But mother (RhD-) is now sensitized to RhD antigen.Fetal –maternal blood transfer during labor
- 7. 2nd Pregnancy- Rapid production of IgG anti-D by mother Maternal IgG anti-D crosses placenta. IgG anti-D attaches to fetal BBCs & marks them for destruction. Fetal or newborn Hemolytic Anemia. Mild case Mild anemia, jaundice Severe Incresed billirubin. CNS damage(kernicterus), death. Father (RhD+) Mother (RhD-) Fetus (RhD+) Repeat encounter with fetal RhD antigen Note: If mother is sensitized to RhD antigen prior to first pregnancy, then first fetus will be affected.
- 9. SIGNS & SYMPTOMS OF RH INCOMPATIBILITY It can cause symptoms ranging from very mild to fatal. Mildest form – Rh Incompatibility: 1. Hemolysis 2. Jaundice 3. Total body swelling 4. Respiratory distress 5. Circulatory collapse 6. Kernicterus 7. It occurs several days after delivery and is characterized initially by- A. Poor feeding B. Decreased activity
- 10. DIAGNOSTIC TESTS MATERNAL BLOOD- The Kleihauer-betke test or flow cytometry Indirect coombs test FETAL BLOOD- • The direct Coombs test • Blood count • Billirubin(direct & indirect)
- 11. TREATMENT Rh incompatibility is treated with a medicine called Rh immunoglobulin. Treatment for a baby who has hemolytic anemia will vary based on the severity of the condition. Goals of Treatment The goals of treating Rh incompatibility are to ensure that baby is healthy and to lower mother’s risk for the condition in future pregnancies. Treatment for Rh Incompatibility If Rh incompatibility is diagnosed during pregnancy, mother will receive Rh immunoglobulin in seventh month of pregnancy and again within 72 hours of delivery. Mother also may receive Rh immunoglobulin if the risk of blood transfer between mother and the baby is high (for example, a miscarriage, ectopic pregnancy, or bleeding during pregnancy).
- 12. Rh immunoglobulin contains Rh antibodies that attach to the Rh-positive blood cells in mother’s blood. When this happens, mother’s body doesn't react to the baby's Rh- positive cells as a foreign substance. As a result, mother’s body doesn't make Rh antibodies. Rh immunoglobulin must be given at the correct times to work properly. Once mother have formed Rh antibodies, the medicine will no longer help. That's why a woman who has Rh-negative blood must be treated with the medicine with each pregnancy or any other event that allows her blood to mix with Rh-positive blood. Rh immunoglobulin is injected into the muscle of arm or buttock. Side effects may include soreness at the injection site and a slight fever. The medicine also may be injected into a vein.
- 13. SCREENING & PREVENTION Rh incompatibility can be prevented with Rh immunoglobulin, as long as the medicine is given at the correct times. Once mother has formed Rh antibodies, the medicine will no longer help. Thus, a woman who has Rh-negative blood must be treated with Rh immunoglobulin during and after each pregnancy or after any other event that allows her blood to mix with Rh- positive blood. Early prenatal care also can help prevent some of the problems linked to Rh incompatibility. For example, doctor can find out early whether mother is at risk for the condition. If mother is at risk, doctor can closely monitor pregnancy. He or she will watch for signs of hemolytic anemia in baby and provided treatment as needed.
- 14. PLEASE LIKE , SHARE AND FOLLOW
