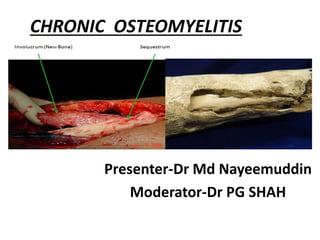
Chronic osteomyelitis
- 1. CHRONIC OSTEOMYELITIS Presenter-Dr Md Nayeemuddin Moderator-Dr PG SHAH
- 2. INTRODUCTION • In pre antibiotic era mortality and morbidity following osteomyelitis was very high. • Antimicrobials drugs have changed the course of osteomyelitis but in developing and under developed countries , where health care facilities are inadequate ,osteomyelitis remains a problem.
- 3. Reason for such a situation(4 failures). • Failure to suspect correct diagnosis within the first 3 – 4 days of onset due to lack of a “high index of suspicion”. • Failure to perform the simple clinical investigations which can confirm the suspicion. • Failure to initiate properly planned therapeutic program. • Failure to continue treatment till the disease is eliminated.
- 4. INTRODUCTION (Contd). • Hematogenous osteomyelitis is the generic name for a whole spectrum of clinical manifestations , the cause of which is infection of bone and marrow from circulating organisms in the blood from distant source. • The infection can be acute , subacute and chronic osteomyelitis depending on the nature , virulence and dose of the infecting organisms , the age , immune system and general condition of host.
- 5. INTRODUCTION (Contd) • ACUTE OSTEOMYELITIS – produces the signs of systemic and local infection • SUBACUTE OSTEOMYELITIS – does not show signs of systemic involvement though local signs are there • CHRONIC OSTEOMYELITIS – presents with discharging sinus and recurrent infections.
- 6. PATHOLOGY • In any infection of bone , there is an attempt at repair that ,if incomplete it results in chronic persistence of infection. • This repair is accomplised by hyperemia of the surrounding tissue , which effects the decalcification of the bone. • Granulation tissue forms and carries in osteoclasts n osteoblasts.
- 7. PATHOLOGY(contd). • Necrotic cancellous bone is readily absorbed and replaced by new bone. • Dead cortex is gradually absorbed about its surface and is detached from living bone to form a sequestrum.(this requires several months) • SEQUESTRUM – is a piece of dead bone , surrounded by infected granulation tissue trying to “eat” the sequestrum away. It appears pale having smooth inner surface and a rough outer.
- 8. Different types of SEQUESTRA TYPE DISEASE TUBULAR PYOGENIC RING EXTERNAL FIXATORS BLACK ACTINOMYCOSIS CORALLIFORM PERTHE’S DISEASE COKE TUBERCULOSIS SANDY TUBERCULOSIS FEATHERY SYPHILIS
- 9. PATHOLOGY (Contd) • When SEQUESTRUM IS COMPLETE, it lies in the free cavity and is LESS attacked by granulation tissue and is absorbed more slowly. • Meanwhile , the surrounding living bone attempts to wall off the infection by forming a thick , dense wall , the INVOLUCRUM. • (INVOLUCRUM is the dense sclerotic bone overlying the sequestrum). • An involucrum usually has multiple openings , the cloacae , through which exudate , bone debris , and sequestra find exit and pass through sinus tracts to the surface.
- 10. Pathology (contd). • CONSTANT DESTRUCTION of neighboring soft tissue leads to THIN skin which is easily traumatised , skin epithelium grows inwards to line the sinus tract. • In chronic osteomyelitis of long standing , multiple cavities and sequestra exist throughout the bone • The shaft becomes thickened , irregular and deformed.
- 13. BACTERIOLOGY • STAPHLOCOCCUS AUREUS ,is the most common infecting organism. • Other organisms are – group A streptococci , pseudomonas aeruginosa , proteus , E.coli , staphylococcus epidermidis . • Hemophilus influenzae – culprit in childrens below 2 years of age. • Bacteroids. • Salmonella in patients suffering from sickle cell anaemia.
- 16. CLINICAL PICTURE • During the period of inactivity no symptoms are present. • The bone is misshapen and the shin is dusky ,thin , scarred and poorly nourished. • A break in the skin causes an ulceration that is slow to heal. • Muscles are scarred and cause contractures of the adjacent joints.
- 17. CLINICAL PICTURE(contd) • Pain is aching type and usually worsens in the night. • The overlying soft tissues become swollen , edematous , warm , reddened and tender. • As the infection progresses a sinus is formed n is drained indefinitely. • Spontaneous closure of the sinus and subsidence of infection often occur following explusion of large fragment.
- 18. CLINICAL PICTURE(contd) • Recurrent flare ups occurs indefinitely over a period of months and years . A sinus may drain continously. • Recurrent toxemia over a long period will causes amyloidosis.
- 19. DIAGNOSIS • The diagnosis is based on Clinical , Laboratory and Imaging studies. • The “GOLD STANDARD” is to obtain a biopsy specimen for histological and microbiological evaluation of the infected bone.
- 20. CLINICAL • Physical examination should be focused on integrity of skin and soft tissue . • Determination of area of tenderness. • Assessing bone stability. • And evaluation of neuro vascular status of the limb
- 21. LABORATORY • Lab studies generally are nonspecific and give no indication for severity of the infection. • ESR and C- Reactive protein are elevated in most patients. • But WBC’S elevated in only 35%.
- 22. Multiple imaging technique are available to evaluate chronic osteomyelitis ,however no technique can absolutely confirm or exclude presence of osteomyelitis. • Imaging should be done to confirm the diagnosis and prepare for surgery. • Initial plain radiographs to be performed it yields valuable info . • Signs of cortical destruction and periosteal reaction strongly suggest the diagnosis of osteomyelitis.
- 23. • Sinography can be preformed if a sinus track is present and can be valuable adjunct to surgical planning. • Isotopic bone scanning is more useful in acute osteomyelitis than chronic osteomyelitis. • CT provides excellent definition of cortical bone and a fair evaluation of the surrounding soft tissues and is especially useful in identifying sequestra. • MRI provides a fairly accurate measure of pathological insult to bone and soft tissue , so it is superior to CT in soft tissue evaluation. • MRI may reveal a well defined rim of high signal intensity surrounding the focus of active disease (RIM SIGN).
- 24. TREATMENT • Requires a multi faceted approach. • In addition to antibiotic and surgical debridement n reconstruction. • 1st objective is removal of dead bones(sequestrum). • 2nd objective is to find a method of obliterating any dead space left after debridement. • 3rd objective is to obtain soft tissue coverage of exposed bone which is a part of the objective of the obliterating dead space.
- 25. TREATMENT(contd). • In spite of somewhat clear objectives, the actual decision making process is not always easy or clear cut. • The real test of a surgeon’s judgement lies not only in deciding when to operate , but also how to avoid meddlesome surgery. • Total eradication of all areas of potentially infected bone is hardly possible.
- 26. TREATMENT(contd). • Surgery for osteomyelitis consists of sequestrectomy and resection of scarred and infected bone and soft tissue. • Ring External fixators are generally used for soft tissue and dead space management after radical debridement. • The GOAL of surgery is to eradicate infection by achieving a viable and vascular environment. • Extensive debridement creates a large dead space – this is treated with ANTIBIOTIC POLYMETHYL METH ACRYLATE (PMMA) beads that fills the dead space and prevents recurrences.
- 27. TREATMENT(contd). • The duration of post operative antibiotics is controversial . • Traditionally , a 6 week course of intravenous antibiotics is prescribed after surgical debridement.
- 28. TREATMENT(contd). • The methods to eliminate the dead space are – 1. Bone grafting with primary and secondary closure. 2. Use of PMMA as a temporary filler of dead space. 3. Local muscle flaps and skin grafting with or without bone grafting. 4. Microvascular transfer of muscle , osseous flaps. 5. The use of bone transport (ILIZAROV TECHNIQUE).
- 29. TREATMENT(contd). • SEQUESTRECTOMY AND CURETTAGE FOR CHRONIC OSTEOMYELITIS SEQUESTRECTOMY means removal of the sequestrum .if it lies within the medullary cavity , a window is made in the overlying involucrum and the sequestrum removed . One must wait for adequate involucrum formation before performing sequestrectomy.
- 30. SEQUESTRECTOMY AND CURETTAGE FOR CHRONIC OSTEOMYELITIS. • Sequestrectomy and curettage require more time to perform and result in considerably more blood loss than an inexperienced surgeon would anticipate. • Sinus tracks can be injected with methylene blue 24 hours before surgery to make them easier to locate and excise.
- 31. OPEN BONE GRAFTING • Papineau et al described an open bone grafting technique for the treatment of chronic osteomyelitis . • This procedure relies on the formation of healthy granulation tissue in a bed of bone graft that will become rapidly vascularised. • The granulation tissue resists infection and is allowed to adequately drained. • This technique is used when free flaps or soft tissue transfer options are limited because of anatomic location .
- 32. OPEN BONE GRAFTING (contd) • Archdeacon and messerschmitt described a modification of the papineau technique using a vaccum assisted closure (VAC). • VAC helps in decreasing the edema and for the closure of soft tissue dead space. • It also promotes the formation of granulation tissue.
- 33. POLYMETHYLMETHACRYLATE ANTIBIOTIC BEAD CHAINS • IT IS COMMONLY USED. • Studies have shown that the local concentrations achieved are 200 times more than intravenous. • High concentration can be achieved by primary closure of the wound. • Short term (10 days), long term(80days) , permanent implantation of PMMA beads is possible.
- 34. BIODEGRADABLE ANTIBIOTIC DELIVERY SYSTEM • It offers a significant advantage over PMMA in that a second procedure is not required to remove the implant. • It is useful when bone stability is not an issue and soft tissue coverage is adequate. • Many manufacturers produce a variety of bioabsorbable substrates(calcium sulfate or calcium phosphate)that can be mixed with antibiotics like vancomycin and tobramycin). • Its still under study.
- 36. SOFT TISSUE TRANSFER • It is mainly done to fill dead space which is left behind after extensive debridement. • Success rate reported in the literature ranges from 66% to 100%. • For eg chronic osteomyelitis of tibia a local muscle graft from gastrocnemius or soleus is used for transfer.
- 37. ILIZAROV TECHNIQUE • This technique allows radical resection of the infected bone • A corticotomy is performed through the normal bone proximal and distal to the area of the disease. • Disadvantage is – long time to achieve solid unioun and high chances of infections. • The treatment of segmental defects of upto 13cms can be achieved.
- 38. ADJUNCTIVE THERAPIES • Hyperbaric Oxygen is not reliably effective but is used as more traditional methods of treatment. • Bone morphogenic proteins (BMPs) and even Platelet Rich Plasmas (PRPs) have been advocated as it has the ability to acccelerate or enchance osteogenesis.
- 39. COMPLICATIONS • An acute exacerbation of the infections occurs commonly. • Growth Abnormalities : shortening –if growth plate is damaged. Lengthening – coz of increased vasularity of the growth plate due to near by osteomyelitis. • Pathologic fracture . • Joint stiffness – may occur because of scarring of soft tissues around the joint. • Sinus tract malignancy – rare complication (squamous cell carcinoma) • Muscle contracture. • Epithelioma. • Amyloidosis.
