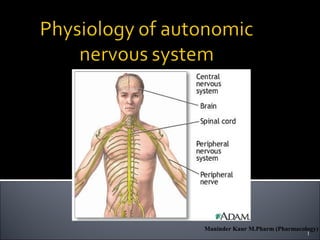
physiology of Autonomic nervous system
- 1. 1 Maninder Kaur M.Pharm (Pharmacology)
- 2. The autonomic nervous system is the subdivision of the peripheral nervous system that regulates body activities that are generally not under conscious control Visceral motor innervates non-skeletal (non- somatic) muscles Visceral sensory will be covered later 2Maninder Kaur M.Pharm (Pharmacology)
- 3. 3Maninder Kaur M.Pharm (Pharmacology)
- 4. 4 Diagram of Autonomic nervous system Diagram contrasts somatic (lower) and autonomic: autonomic somatic this dorsal root ganglion is sensory Maninder Kaur M.Pharm (Pharmacology)
- 5. Neurotransmission in ANS occurs in 5 steps: • Impulse conduction. • Neurotransmitter release. • Activity on pre- ganglionic neurons. • Activity on post- ganglionic neurons. • Termination of neurotransmitter release. 5 Maninder Kaur M.Pharm (Pharmacology)
- 6. Parasympathetic division Sympathetic division Parasympathetic: routine maintenance. “rest &digest” Sympathetic: mobilization & increased metabolism. “fight, flight or fright” 6Maninder Kaur M.Pharm (Pharmacology)
- 7. 2 divisions: Sympathetic ▪ “Fight or flight” ▪ “E” division ▪ Exercise, excitement, emergency, and embarrassment Parasympathetic ▪ “Rest and digest” ▪ “D” division ▪ Digestion, defecation, and diuresis 7Maninder Kaur M.Pharm (Pharmacology)
- 8. 8 Also called the craniosacral system because all its preganglionic neurons are in the brain stem or sacral levels of the spinal cord. Cranial nerves III,VII, IX and X In lateral horn of gray matter from S2-S4 Only innervate internal organs (not skin). Acetylcholine is neurotransmitter at end organ as well as at preganglionic synapse: “cholinergic”. Maninder Kaur M.Pharm (Pharmacology)
- 9. Works to save energy, aids in digestion, and supports restorative, resting body functions. Decrease in heart rate Increased gastro intestinal tract tone and peristalsis Urinary sphincter relaxation Vasodilation – decrease in blood pressure 9Maninder Kaur M.Pharm (Pharmacology)
- 10. 10Maninder Kaur M.Pharm (Pharmacology)
- 11. 11Maninder Kaur M.Pharm (Pharmacology)
- 12. 12Maninder Kaur M.Pharm (Pharmacology)
- 13. 13Maninder Kaur M.Pharm (Pharmacology)
- 14. Location of cholinergic receptors- 1. Postganglionic parasympathetic neuroeffector junctions. 2. All autonomic ganglia. 3. At the neuromuscular endplate. 14Maninder Kaur M.Pharm (Pharmacology)
- 15. Two types of receptors are present- Muscarinic receptor. Nicotinic receptor. 15Maninder Kaur M.Pharm (Pharmacology)
- 16. M-cholinoceptors can be classified into subtypes according to their molecular structure, signal transduction, and ligand affinity in the M1, M2, M3 subtypes etc. • M1-receptors are present on nerve cells, e.g., in ganglia, where they mediate a facilitation of impulse transmission from preganglionic axon terminals to ganglion cells. • M2-receptors mediate acetylcholine effects on the heart. Opening of K+ channels leads to slowing of diastolic depolarization in sinoatrial pacemaker cells and a decrease in heart rate. 16Maninder Kaur M.Pharm (Pharmacology)
- 17. M3-receptors are found in the glandular epithelia (which respond with activation of phospholipase C and increases secretory activity) and in smooth muscle. 17 Maninder Kaur M.Pharm (Pharmacology)
- 18. Muscarinic receptor (G protein-linked: 7 subunits) 18 Maninder Kaur M.Pharm (Pharmacology)
- 19. NM -cholinoceptors Location: neuromuscular junction. Function: depolarization of muscle end plate and contraction of skeletal muscle. NN -cholinoceptors Location: autonomic ganglia. Function: depolarization postganglionic membrane (in adrenal medulla – catecholamine release). 19Maninder Kaur M.Pharm (Pharmacology)
- 20. 20 Maninder Kaur M.Pharm (Pharmacology)
- 21. (1) Choline ester (stimulants of M- and N- receptors): Acetylcholine, Carbachol, etc. (2) Alkaloids a) stimulants of M-receptors: ▪ Pilocarpine, Cevimeline (dry mouth), ▪ Bethanechole, Musacarine, Phalloidin b) stimulants of N-receptors: ▪ Nicotine, Cytisine (Tabex® ), Lobeline 21Maninder Kaur M.Pharm (Pharmacology)
- 22. (1) Reversible drugs (most are carbamates) a) With N3+ (cross BBB) Alkaloids: Galantamine, Physostigmine Synthetic drugs: Donepezil, Rivastigmine, Tacrine. b) With N4+ (do not cross BBB)- Demecarium, Edrophonium (Tensilon® ),Neostigmine, Pyridostigmine. 22Maninder Kaur M.Pharm (Pharmacology)
- 23. (2) Irreversible anticholinesterase agents (most of them are organophosphates)- a) Thiophosphate insecticides Parathion Malathion (Pedilin® – in pediculosis) b) Nerve paralytic gases for chemical warfare Tabun Sarin Soman 23Maninder Kaur M.Pharm (Pharmacology)
- 24. cardiac output M2: decreases SA node: heart rate (chronotropic) M2: decreases cardiac muscle: contractility (inotropic) M2: decreases (atria only) conduction at AV node M2: decreases smooth muscles of bronchioles M3: contracts pupil of eye M3: contracts ciliary muscle M3: contracts salivary glands: secretions stimulates watery secretions GI tract motility M1, M3: increases smooth muscles of GI tract M3: contracts sphincters of GI tract M3: relaxes glands of GI tract M3: secretes 24Maninder Kaur M.Pharm (Pharmacology)
- 25. Myasthenia gravis. Belladonna poisoning. In glucoma 25Maninder Kaur M.Pharm (Pharmacology)
- 26. These are drugs which oppose the acetylcholine actions or block the cholinergic receptors. Anti- cholinergics mainly block the muscarinic receptor. 26Maninder Kaur M.Pharm (Pharmacology)
- 27. Atropine, the prototype drug of this class, is a highly selective blocking agent for pre and post muscarinic receptors, but some of its synthetic derivatives have significant nicotinic blocking property as well. 27Maninder Kaur M.Pharm (Pharmacology)
- 28. 1. Natural alkaloids: Atropine (spasmolytic, mydriatic), Hyoscine (Scopolamine), Scopoderm® TTS (antiemetic) 2. Semisynthetic derivatives • Mydriatics: Homatropine • GI spasmolytics: Hyoscine butyl bromide (Buscolysin® ) 28Maninder Kaur M.Pharm (Pharmacology)
- 29. 3. Synthetic compounds • GI spasmolytics: Oxyphenonium • Antiulcus drugs: Pirenzepine (M1-blockers) • Antiasthmatics: Ipratropium and Tiotropium • Antidisurics: Flavoxate, Oxybutynyne, Trospium • Mydriatics: Tropicamide • Antiparkinsonian (central M-cholinolytics): ▪ Benztropine, Biperiden, Trihexyphenidyl 29Maninder Kaur M.Pharm (Pharmacology)
- 30. 30Maninder Kaur M.Pharm (Pharmacology)
- 31. Atropine (-) 31Maninder Kaur M.Pharm (Pharmacology)
- 32. • CNS. Atropine has an overall stimulant action. Its stimulant effects are not appreciable at low doses which produce peripheral effects because of restricted entry into the brain. • Atropine stimulates many medullar centers- vagal, respiratory, and vasоmotor. • By blocking the relative cholinergic overactivity in basal ganglia, it suppresses tremor and rigidity in parkinsonism. • High doses cause cortical excitation, rest- lessness, disorientation, hallucinations. 32Maninder Kaur M.Pharm (Pharmacology)
- 33. CVS. Atropine causes tachycardia, due to blockade of M2- receptors on SA node through which vagal tone decreases HR. Atropine does not influence BP. It blocks the vasodepressor action of cholinergic agonists. Eye. Topical instillation of atropine (0.1%) causes mydriasis, abolition of light reflex, and cycloplegia, lasting 7–10 days. This results in photophobia and blurring of near vision. The intraocular tension rises, specially in narrow angle glaucoma, but conventional systemic doses produce minor ocular effects. 33Maninder Kaur M.Pharm (Pharmacology)
- 34. Smooth muscles. All visceral smooth muscles with parasympathetic inervation are relaxed (M3 blokade).Tone and amplitude of GIT are reduced. Spasm may be reduced, constipation may occur. Peristalsis is only incompletely suppressed because it is primarily regulated by local reflexes and other neurotransmitters (serotonin, encephalin, etc.). Atropine causes bronchodilation and reduced airway resistance, especially in asthma patients. 34Maninder Kaur M.Pharm (Pharmacology)
- 35. Glands. Atropine decreases sweat, salivary, tracheo- bronchial, and lacrimal secretion (M3-blockade). Skin and eyes become dry, talking, and swallowing my be very difficult. Atropine decreases less the secretion of acid and pep-sin and more of the mucus in the stomach. Body temperature. Rise in body temperature occurs at higher doses, and is due to both inhibition of sweating as well as stimulation of the temperature regulating centre in the hypothalamus. 35Maninder Kaur M.Pharm (Pharmacology)
- 36. saliva, sweat, bronchial secretion > eye > bronchial muscles > heart > intestinal and bladder smooth muscles > gastric glands and gastric smooth muscles 36Maninder Kaur M.Pharm (Pharmacology)
- 37. NEUROMUSCULAR BLOCKING AGENTS: Skeletal muscle relaxants act peripherally at neuromuscular junction. According to their action they are divided into the following groups. •Nondepolarizing (competitive) agents or curare-like drugs •Depolarizing (hyperdepolarazing) agents 37Maninder Kaur M.Pharm (Pharmacology)
- 38. Also called thoracolumbar system: all its neurons are in lateral horn of gray matter from T1-L2 Lead to every part of the body Easy to remember that when nervous, you sweat; when afraid, hair stands on end; when excited blood pressure rises (vasoconstriction): these sympathetic only Also causes: dry mouth, pupils to dilate, increased heart & respiratory rates to increase O2 to skeletal muscles, and liver to release glucose Norepinephrine (noradrenaline) is neurotransmitter released by most postganglionic fibers (acetylcholine in preganglionic): “adrenergic” 38Maninder Kaur M.Pharm (Pharmacology)
- 39. Helps the body cope with external stimuli and functions during stress (triggers the flight or fight response) Vasoconstriction – increase in blood pressure Increased heart rate Increased respiratory rate Cold, sweaty palms Pupil dilation 39Maninder Kaur M.Pharm (Pharmacology)
- 40. 40Maninder Kaur M.Pharm (Pharmacology)
- 41. 41Maninder Kaur M.Pharm (Pharmacology)
- 42. Sympathetic and parasympathetic divisions typically function in opposition to each other. But this opposition is better termed complementary in nature rather than antagonistic. For an analogy, one may think of the sympathetic division as the accelerator and the parasympathetic division as the brake. The sympathetic division typically functions in actions requiring quick responses. The parasympathetic division functions with actions that do not require immediate reaction. Consider sympathetic as "fight or flight" and parasympathetic as "rest and digest". 42Maninder Kaur M.Pharm (Pharmacology)
- 43. END 43
